May 10, 2021, by School of Medicine
30 at 30: The career of Anna Kent
Working within international humanitarian medical aid became a life goal of mine as I grew up. As many of us are, I was appalled to learn of the social and health inequalities across the world and wanted to make a positive difference.
In 1999, aged 18, I was privileged to join one of the first cohorts for an Undergraduate Masters’ Degree in Nursing at The University of Nottingham (UoN). This was a very progressive course for its era, with simultaneous academic lectures and practical placements to become a Registered Nurse. A core philosophy of our study was ‘evidenced-based practice’ which, at the time, was still an emerging concept within clinical nursing practice. We were encouraged to undertake our own empirical research as part of our studies, enabling us to critically review the research of others, and then apply our own findings to contemporary nursing practice.
I took these clinical and academic skills to first work within acute and emergency hospital care as a nurse in a busy Emergency Department (ED) at Queen’s Medical Centre (QMC) in Nottingham. Following this, I joined Médecins Sans Frontières (MSF) – Doctors without Borders – a medical organisation that sends volunteer doctors, nurses and other professionals to conflict zones, natural disasters and epidemics.
 My first mission for MSF was a year in South Sudan, a country torn apart by civil war. We found the need to be enormous as conflict had destroyed any reliable access to health care and education, and millions of people had been displaced from their homes due to violence. I drew on every aspect of the nursing education I had gained at the UoN, needing to apply my knowledge within a completely different and fast-changing context. With the absence of electricity and running water, we were often working without access to basic medical tests such as ultrasounds, X-rays or even baseline blood tests. My basic anatomy and physiology knowledge, which I learnt at the UoN, had never been so crucial to help save lives. Despite running a basic health care unit from a very humble structure, just four mud huts, we were able to save the lives of most of the 500-1000 people that came to us each month. This was because we had knowledge, access to good quality medications, and could airlift people out who needed emergency surgery, or a caesarean section. After an unexpected, but successful, delivery of triplets I knew I wanted to learn more about midwifery.
My first mission for MSF was a year in South Sudan, a country torn apart by civil war. We found the need to be enormous as conflict had destroyed any reliable access to health care and education, and millions of people had been displaced from their homes due to violence. I drew on every aspect of the nursing education I had gained at the UoN, needing to apply my knowledge within a completely different and fast-changing context. With the absence of electricity and running water, we were often working without access to basic medical tests such as ultrasounds, X-rays or even baseline blood tests. My basic anatomy and physiology knowledge, which I learnt at the UoN, had never been so crucial to help save lives. Despite running a basic health care unit from a very humble structure, just four mud huts, we were able to save the lives of most of the 500-1000 people that came to us each month. This was because we had knowledge, access to good quality medications, and could airlift people out who needed emergency surgery, or a caesarean section. After an unexpected, but successful, delivery of triplets I knew I wanted to learn more about midwifery.
In 2008, I returned to the UoN to gain my First Degree in Midwifery, following which I worked on the busy delivery unit at QMC whilst continuing to work as a nurse in ED.
My desire to work within humanitarian aid continued and I did a further two missions with MSF. One was in Haiti following the earthquake of 2010 and subsequent cholera outbreak. Here, I put into action the philosophy of ‘evidence-based practice’ as we helped to create the first specific obstetric guidelines when working within a cholera epidemic.
 Following this, I spent nearly a year providing health care for a refugee camp in Bangladesh, with the clinical responsibility for all female and pregnancy health in a Rohingya refugee camp of 30,000 people. The Rohingya people I met had fled persecution in Myanmar and were extremely vulnerable, marginalised and unable to otherwise access basic health care or mental health support. I had to draw on every element of my education from the UoN, from both of my qualifications, as the clinical work was so extreme and the humanitarian situation so desperate. I was able to create a birth unit and employ and train Bangladeshi nurses to become midwives; this went some way to making pregnancy and childbirth safer for the Rohingya women I was honoured to meet. However, with over 1 million Rohingya people having now fled to Bangladesh alone, the situation for them remains extreme and many still suffer unimaginable hardship.
Following this, I spent nearly a year providing health care for a refugee camp in Bangladesh, with the clinical responsibility for all female and pregnancy health in a Rohingya refugee camp of 30,000 people. The Rohingya people I met had fled persecution in Myanmar and were extremely vulnerable, marginalised and unable to otherwise access basic health care or mental health support. I had to draw on every element of my education from the UoN, from both of my qualifications, as the clinical work was so extreme and the humanitarian situation so desperate. I was able to create a birth unit and employ and train Bangladeshi nurses to become midwives; this went some way to making pregnancy and childbirth safer for the Rohingya women I was honoured to meet. However, with over 1 million Rohingya people having now fled to Bangladesh alone, the situation for them remains extreme and many still suffer unimaginable hardship.
 After retiring from frontline humanitarian aid work, I returned to the UoN to teach on several different modules. In 2012, I was fortunate to be selected as a ‘Gamesmaker’ for the Olympic and Paralympic Games held in London. My role as a nurse was mainly based within the Olympic Stadium where I was able to respond to an array of medical and surgical emergencies, but also have moments to enjoy The Games.
After retiring from frontline humanitarian aid work, I returned to the UoN to teach on several different modules. In 2012, I was fortunate to be selected as a ‘Gamesmaker’ for the Olympic and Paralympic Games held in London. My role as a nurse was mainly based within the Olympic Stadium where I was able to respond to an array of medical and surgical emergencies, but also have moments to enjoy The Games.
In 2014, I was honoured to be awarded a Graduate Laureate from the UoN, in recognition of my international humanitarian aid work. Following this, in 2015, I returned to Bangladesh to teach clinical skills on the first ever midwifery course for that country. This was very humbling to be part of, though my personal role was minor, as it was a major social change – for the first time, midwifery was being formally recognised in Bangladesh as an autonomous profession in its own right. It was so satisfying to take the education I learnt at the UoN and teach student midwives in Bangladesh, and I have followed their progression and seen them go on to graduate. It’s wonderful to know they will save the lives of countless women in their future careers.
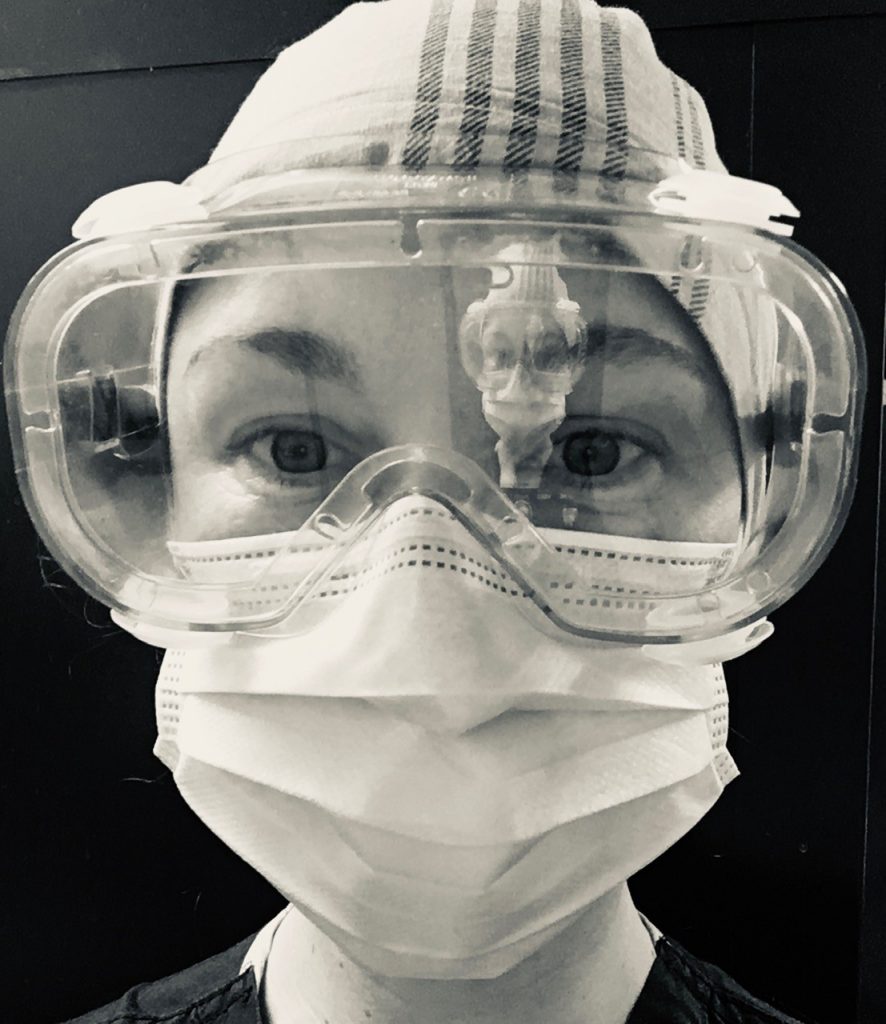 Over the last year, 2020/2021, I have relied again on my core nursing and midwifery education from the UoN as I have worked ‘frontline’ in the NHS throughout the whole of the Covid-19 pandemic. Evidence-based practice has remained at the forefront of my clinical practice over these last few months, challenging us all in the NHS in new ways, as we have had to learn and adapt at speed to the changing context. My current roles in the NHS are as an acute cardiology nurse and a hospital midwife at Dorset County Hospital: a job combination which may seem unusual but is perfect for me in combining all the elements of my education, experience and passion.
Over the last year, 2020/2021, I have relied again on my core nursing and midwifery education from the UoN as I have worked ‘frontline’ in the NHS throughout the whole of the Covid-19 pandemic. Evidence-based practice has remained at the forefront of my clinical practice over these last few months, challenging us all in the NHS in new ways, as we have had to learn and adapt at speed to the changing context. My current roles in the NHS are as an acute cardiology nurse and a hospital midwife at Dorset County Hospital: a job combination which may seem unusual but is perfect for me in combining all the elements of my education, experience and passion.
I’m so thankful for all the UoN has offered to me over the years; I have taken these skills to improve the health and lives of the people I have met in both the UK and overseas. It’s exciting to see how education continues to spread over the world in the new cohorts of midwifery students in the UK and Bangladesh, knowing how this knowledge and skill will directly saves the lives of many people in the future.
By Anna Kent – Nottingham Alumni, Masters’ Degree in Nursing and First Degree in Midwifery

Having had the pleasure and honor to work alongside Anna as a midwife, I know that there are many more facets and stories to her incredible career.
Thank you Anna for being so kind, caring and inspirational. There is no way we could possibly count all the lives you have changed and touched on so far.
Anna you are incredible! Haven’t met a more modest, hard working selfless professional. You have endured your own personal tragedy and yet today I learn of such amazing achievements. Your family must be so proud and your little girl has an amazing role model.
Congratulations
Wow Anna you have truly lived life fully, since I last worked with you in A&E. you are a huge inspiration and I am in awe of your devotion to nursing. Well done xxxx
Anna’s professionalism and humanitarianism are only matched by the integrity and charm of her personality.
I can only echo what others have said previously. As a colleague in both Nottingham’s QMC A & E, and MSF, I know what a very special person Anna is, both professionally and on a personal level. Well done, Anna, for all you have achieved. Interesting to read – I knew so little of that!