August 13, 2021, by School of Medicine
30 at 30: Ye Old Trip to Nottingham: A Contagious Enthusiasm for Nursing
The last time I visited Nottingham from San Francisco, it was to present the film “5B” about the AIDS unit at San Francisco General Hospital where I first worked in 1987. It was timed to coincide with World AIDS Day 2019, 1 December. Unbeknownst to us, another novel virus emerged that same month. Tragic and fitting, as I began my career while HIV emerged in the 1980’s. Since that time, I have cared for people with HIV and tuberculosis and visited the homes of people with SARS and now COVID-19.
In 2003, I went to the homes of San Francisco residents to obtain nasopharyngeal swabs and ask them to quarantine. As I fumbled my way into the protective kit in the apartment hallway, I remember being terrified of getting SARS and transmitting it to my partner and children. After all, one of my colleagues contracted HIV from an intravenous needle injury and I became infected with tuberculosis shortly after caring for a patient with both AIDS and tuberculosis. But I reminded myself that I had signed up for this and I walked into the home only to see my fear reflected in the patient’s eyes as they regarded a stranger entering their home in an elaborate “space suit”.
SARS seems to have vanished as fast as it appeared and advances in diagnostics, prevention and treatment have made it reasonable to envision a world without HIV or tuberculosis. Effective suppression of HIV made it possible for my colleague to live to promote safer devices that are helping to eliminate healthcare associated transmission of HIV, Hepatitis B and other blood-borne pathogens. My doctoral research showed that receiving care for active tuberculosis from San Francisco’s public health system was a protective factor. Public health can be superior to private health care.
Though American nurses and researchers and activists have helped advance caring during pandemics, I have been fascinated by British activist leaders. Florence Nightingale has been practically embalmed as the founder of modern nursing and is sometimes remembered as an innovator in epidemiology. Her efforts to promote public health and improve conditions in colonial India are less widely known. Despite never going there, she recognised how the poor of India were suffering preventable deaths due to imperial policy. Her efforts on behalf of the invisible masses were themselves ignored.
To advocate for patient safety is to advocate for nursing safety and vice versa. There is emerging research that demonstrates the positive association between adequate nursing staffing and decreased patient mortality, for example. With COVID-19, there are numerous examples of how critical it is to prevent infection from being passed among and between patients and hospital staff. In California, as of July 29, local health departments have reported 116,208 confirmed positive cases in health care workers and 481 deaths state-wide. This happened despite California having some of the strongest mandates for safe nurse:patient ratios and aerosolised transmissible disease regulations. England has experienced a per capita incidence of COVID-19 that is somewhat less than California but has sadly suffered many more deaths. With a chronic nursing shortage in both countries it is critical that best practices in safety include evidence-based guidelines.
Evidence-based practice is what brought me to Nottingham to begin with. Thanks to the Florence Nightingale scholarship, Nottingham University Hospitals NHS Trust (NUH) nurse Emma Popejoy travelled around the United States and saw how nurses were implementing evidence-based practice. Her mentor, NUH Assistant Director of Nursing Dr Joanne Cooper, invited me to come and see the exemplary work that she and her colleagues were doing in Nottingham. Having worked in a publicly funded healthcare system, I was fascinated to compare and contrast the San Francisco Department of Public Health with the NUH Trust. San Francisco General Hospital is funded by taxpayers putting it in the minority of U.S. hospitals. I was fascinated by the near-universal support of the NHS when I visited. In my current position as a telephone advice nurse, I endeavour to overcome the reluctance of many patients to let me call an ambulance for them because they are afraid of the bill. At the same time, I am saddened by the immense pressures placed on the NHS to safely recruit and retain nursing staff.
No discussion of evidence-based practice and epidemics can be complete without a visit to Nottingham’s own “Ye Olde Trip to Jerusalem” pub. The evidence that this pub is the oldest in the UK is rather thin but that only demonstrates the need for further research and perhaps another pint. But the reference to the Crusades has particular relevance for this Jewish nurse at this particular time. Why? Because I learned that the effort to “liberate” Jerusalem from Muslims was accompanied by anti-Jewish pogroms throughout Christian Europe. Jews were expelled from England about 100 years after the founding of the pub. But what do the Crusades have to do with pandemics? More than historical and current mistreatment of those who are different, it shows the persistence of war as a metaphor in healthcare. Early 20th century Americans funded tuberculosis treatment with the sale of “Christmas Seals” that featured the Crusader’s Cross.

At the same time, the text is correct: Tuberculosis (and HIV, and COVID 19) indeed steal lives and our work in healthcare is for the protection of all of us.
Literally around the corner from Ye Olde Trip to Jerusalem is a statue of Robin Hood and it’s just a short walk to the caves where Ned Ludd’s rebels hid from the authorities. Nottingham is THE destination for nurses interested in public health, equity and costume drama.
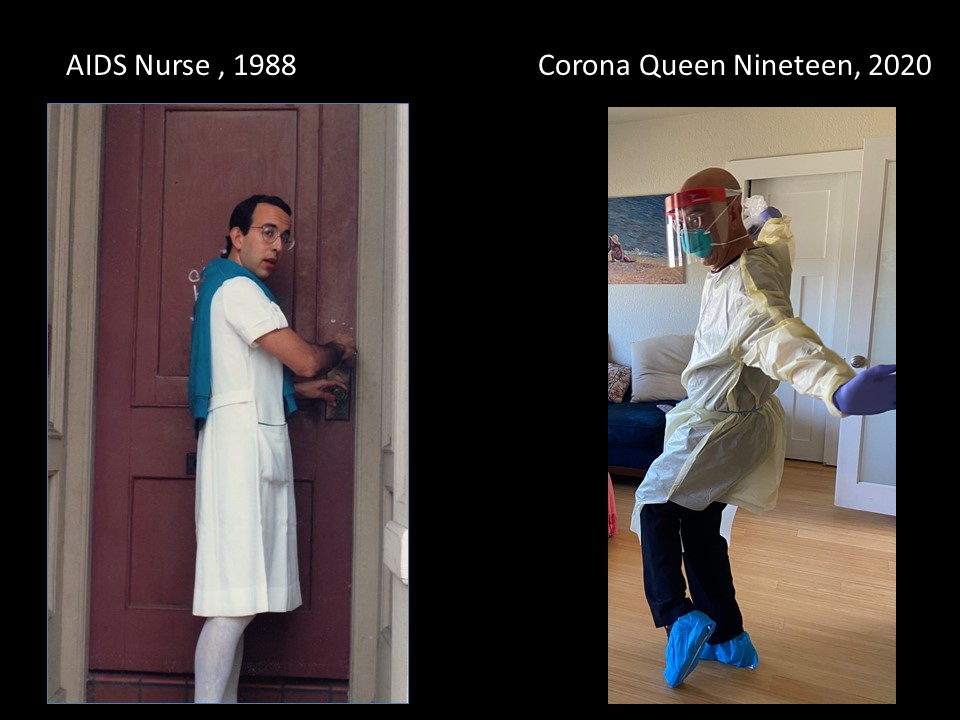
Speaking of fashion history, I presented the 5B film at Queen’s Medical Centre wearing a dress I had purchased more than 30 years prior. As a San Francisco nurse who has had the immense privilege of working with and caring for small case queens such as myself it was both figuratively and literally fitting.
Proper nursing has always relied on science and individualised ethical care. Being kind to patients and ourselves is best practice. For that reason, I was eager to volunteer again when COVID-19 arrive in San Francisco. I didn’t wear heels, or even a dress, when I swabbed the first handful of terrified San Franciscans for the virus. But I did a little dance called “Flatten the Curve” nonetheless and have given myself the drag name “Corona Queen Nineteen”. I can reveal now in this blog exclusively, that there is no choreography nor music as I am a “triple threat” who can neither sing, dance, or act. But I can nurse.
By Sasha Cuttler

Dear, dear, Sasha Cuttler Nurse and Butler…
Many thanks again for your years and years of service and for personally saving my life when we had Covid-19 last year and for always being there!
xxxooo your sib in law
Dr. Sasha Cuttler is worth one hundred health care professionals for the personal and professional benefits he has brought to his colleagues, his patients, and to the institutions that have called upon him.
-Dr. James Magee